
Lansdowne, PA
(610) 626-3338

Lansdowne, PA
(610) 626-3338

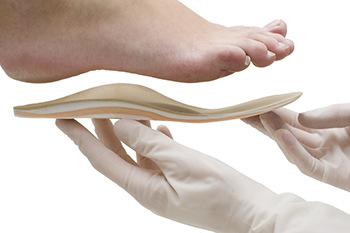
Orthotics, typically associated with seniors or athletes, offer benefits for individuals of all ages, including children. Custom orthotics provide essential support for arches, treat various foot conditions, alleviate general foot pain, and prevent future injuries. Children can significantly benefit from orthotics as they provide a sturdy foundation for developing feet. Timely evaluation and intervention are important for children with foot problems, as their feet grow faster than the rest of their bodies. Orthotics are not recommended for children under 3 years old as many common concerns, such as flat feet or misalignment, tend to resolve naturally during early development. However, signs such as abnormal gait, excessive shoe wear, frequent falls, pain, or deformities may warrant orthotic consultation. Orthotics serve as guides, aiding children in their development by correcting alignment, posture, and balance issues while reducing muscle fatigue. These devices are used to gently realign the foot biomechanically, leading to improved foot function and symptom relief. For active children or those involved in sports, timely orthotic intervention is essential to address gait and mobility issues. Children's orthotics should be replaced every 18 to 24 months due to rapid foot growth. If you suspect your child may benefit from orthotics, it is suggested that you make an appointment with a podiatrist to discuss the potential.
If you are having discomfort in your feet and would like to try orthotics, contact Dr. George Yarnell from Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
What Are Orthotics?
Orthotics are inserts you can place into your shoes to help with a variety of foot problems such as flat feet or foot pain. Orthotics provide relief and comfort for minor foot and heel pain but can’t correct serious biomechanical problems in your feet.
Over-the-Counter Inserts
Orthotics come in a wide variety of over-the-counter inserts that are used to treat foot pain, heel pain, and minor problems. For example, arch supports can be inserted into your shoes to help correct overarched or flat feet, while gel insoles are often used because they provide comfort and relief from foot and heel pain by alleviating pressure.
Prescription Orthotics
If over-the-counter inserts don’t work for you or if you have a more severe foot concern, it is possible to have your podiatrist prescribe custom orthotics. These high-quality inserts are designed to treat problems such as abnormal motion, plantar fasciitis, and severe forms of heel pain. They can even be used to help patients suffering from diabetes by treating foot ulcers and painful calluses and are usually molded to your feet individually, which allows them to provide full support and comfort.
If you are experiencing minor to severe foot or heel pain, it’s recommended to speak with your podiatrist about the possibilities of using orthotics. A podiatrist can determine which type of orthotic is right for you and allow you to take the first steps towards being pain-free.
If you have any questions please contact our office located in Lansdowne, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Ankle foot orthotics are shoe inserts that offer support to control the placement and movement of the ankle, correct deformities, and compensate for weakness. These inserts are used to stabilize the foot and ankle and provide toe clearance during the swing phase of gate.
Athletes often suffer foot problems because their feet are not being supported within the shoe. Ankle and foot orthotics are custom made inserts that alleviate stress on the foot. However custom orthotics should be prescribed by a podiatrist who specializes in customized footwear and orthotics design. These inserts are used by athletes for different reasons. Runners use orthotics to absorb shock at heel contact and to set up the forefoot for push-off. Basketball players wear them to control their forefeet while jumping and running.
The two main types of orthotics are over-the-counter orthotics and custom-made orthotics. To be eligible for custom orthotics, an examination of the foot and ankle will need to be completed. Afterward, both the foot and ankle will need to be casted and fitted for the proper orthotic. When the fitting process is complete, adjustments can be made to make sure everything fits perfectly.
Over the counter orthotics tend to be more popular than custom fit ones. Athletes who have less severe aches and pains in the foot, ankle or lower back area can use the over-the-counter version of orthotics. Unfortunately, over-the-counter orthotics tend to not work in treating severe injuries or ailments. Whenever you suspect you may need an ankle foot orthotic, you should consult with your podiatrist to determine which type of orthotic is right for you.
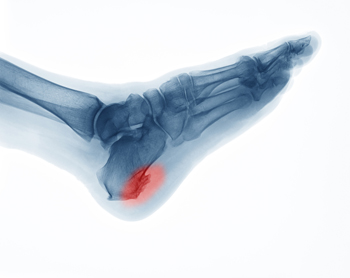
Heel spurs are bony protrusions on the underside of the heel bone that in some cases can cause discomfort and pain. It is generally believed that heel spurs form when calcium deposits accumulate over several months on the calcaneus, or heel bone. However, heel spurs can also be associated with other foot issues, such as plantar fasciitis, where inflammation of the tissue under the foot can contribute to their development. In addition, certain medical conditions like gout, rheumatoid arthritis, and ankylosing spondylitis, all of which damage the joints, can result in heel spurs. Risk factors of heel spurs include having flat feet, engaging in high-impact aerobic exercises, and aging, particularly among people over 62 years old. Obesity, overpronation, and wearing high heels can significantly raise the risk of heel spur development. In fact, younger women tend to have a higher incidence of heel spurs, possibly due to the use of high heels, which can impact foot biomechanics. If you're experiencing heel pain, especially if it's persistent, it's suggested that you make an appointment with a podiatrist for a proper diagnosis and tailored treatment plan.
Heel spurs can be incredibly painful and sometimes may make you unable to participate in physical activities. To get medical care for your heel spurs, contact Dr. George Yarnell from Pennsylvania. Our doctor will do everything possible to treat your condition.
Heels Spurs
Heel spurs are formed by calcium deposits on the back of the foot where the heel is. This can also be caused by small fragments of bone breaking off one section of the foot, attaching onto the back of the foot. Heel spurs can also be bone growth on the back of the foot and may grow in the direction of the arch of the foot.
Older individuals usually suffer from heel spurs and pain sometimes intensifies with age. One of the main condition's spurs are related to is plantar fasciitis.
Pain
The pain associated with spurs is often because of weight placed on the feet. When someone is walking, their entire weight is concentrated on the feet. Bone spurs then have the tendency to affect other bones and tissues around the foot. As the pain continues, the feet will become tender and sensitive over time.
Treatments
There are many ways to treat heel spurs. If one is suffering from heel spurs in conjunction with pain, there are several methods for healing. Medication, surgery, and herbal care are some options.
If you have any questions feel free to contact our office located in Lansdowne, PA . We offer the latest in diagnostic and treatment technology to meet your needs.
Heel spurs are calcium deposits that cause bone protrusions on the heel bone. Heel spurs are usually associated with plantar fasciitis, which occurs when the plantar fasciitis in the foot becomes inflamed. Typically, heel spurs don’t cause any symptoms. However, they can produce chronic or intermittent heel pain. Those who have had the condition often describe the irritation as a stabbing pain.
There are risk factors that may make you more likely to develop heel spurs. People who have abnormal walking gaits, run and jog on hard surfaces, are obese, or wear poorly fitting shoes are more likely to develop heel spurs.
Fortunately, there are precautions you can take to avoid developing heel spurs. One of the best ways to do this is by wearing well-fitting shoes with shock-absorbent soles. Another preventative technique is to choose running shoes if you plan on running, and walking shoes if you plan on walking. Shoes are made for different activities and it is important to research a shoe before you purchase a pair.
The pain associated with heel spurs often decreases the more you walk. However, a recurrence of pain after an extended period of rest or walking is likely to occur with this condition. Those with severe heel spur pain may opt to go the surgical route for treatment. However, more than 90% of those with the condition get better without surgical treatment. If you have a heel spur and want to know if surgery is right for you, you should go to your podiatrist and he or she will be able to conduct a pre-surgical test or exam to determine if you are an optimal candidate for surgery.
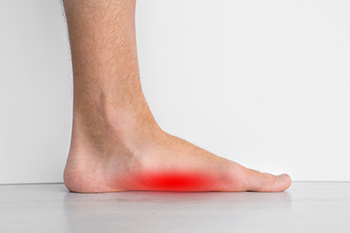
Flat feet, resulting from a collapsed arch, can lead to pain and discomfort, affecting both children and adults. When non-surgical approaches fall short, surgical intervention offers a viable solution. Surgery for flat feet aims to reconstruct the foot's architecture to restore a supportive arch and alleviate complications like change of gait, knee pain, plantar fasciitis, and Achilles tendonitis. An evaluation before surgery involves a thorough history, examination, and imaging. Surgical intervention may involve tendon reconstruction, bone augmentation, joint fusion, or bone resection. Post-surgery recovery may take up to four months and requires keeping the weight off the affected foot as well as taking prescribed pain relief medication. A protective cast or boot may be needed. Surgical treatment for flat feet, while not necessary in many cases, offers an opportunity to regain mobility, alleviate pain, and enhance overall quality of life. To find out if surgery for flat feet is right for you, it is suggested that you make an appointment with a podiatrist for a full examination.
Flatfoot is a condition many people suffer from. If you have flat feet, contact Dr. George Yarnell from Pennsylvania. Our doctor will treat your foot and ankle needs.
What Are Flat Feet?
Flatfoot is a condition in which the arch of the foot is depressed and the sole of the foot is almost completely in contact with the ground. About 20-30% of the population generally has flat feet because their arches never formed during growth.
Conditions & Problems:
Having flat feet makes it difficult to run or walk because of the stress placed on the ankles.
Alignment – The general alignment of your legs can be disrupted, because the ankles move inward which can cause major discomfort.
Knees – If you have complications with your knees, flat feet can be a contributor to arthritis in that area.
Symptoms
Treatment
If you are experiencing pain and stress on the foot you may weaken the posterior tibial tendon, which runs around the inside of the ankle.
If you have any questions please feel free to contact our office located in Lansdowne, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Flatfoot is a foot disorder that is not as straightforward as many people believe. Various types of flatfoot exist, each with their own varying deformities and symptoms. The partial or total collapse of the arch, however, is a characteristic common to all types of flatfoot. Other signs of flatfoot include:
One of the most common types of flatfoot is flexible flatfoot. This variation usually starts in childhood and progresses as one ages into adulthood. Flexible flatfoot presents as a foot that is flat when standing, or weight-bearing. When not standing, the arch returns. Symptoms of flexible flatfoot include:
Your podiatrist will most likely diagnose flatfoot by examining your feet when you stand and sit. X-rays may be taken to define the severity and help determine the treatment option best for your condition. Nonsurgical treatments can include activity modification, weight loss, orthotics, immobilization, medications, physical therapy, shoe modifications, and ankle foot orthoses (AFO) devices. If nonsurgical methods prove ineffective, surgery may be considered. Multiple surgical procedures can correct flatfoot; and depending on your specific condition, one may be selected alone or combined with other techniques to ensure optimal results.
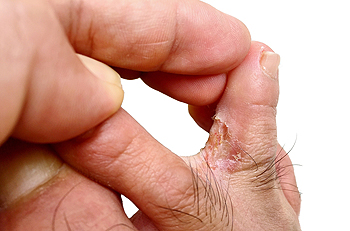
Athlete's foot, medically known as tinea pedis, is a common fungal infection affecting the feet and causing itchy, red, and flaky rashes. This condition, despite its name, can affect anyone not just athletes. It thrives in warm, humid conditions like sweaty feet inside poorly ventilated shoes or walking barefoot in locker rooms or by pool areas. Symptoms can include a rash, itching, skin cracking, and burning sensations, often affecting the area between the fourth and fifth toes. Risk factors include closed shoes, excessive foot sweating, poor hygiene, living in warm environments, and weakened immune systems. Men are more susceptible to athlete’s foot than women. Diagnosis relies on typical symptoms, but tests may be necessary in uncertain cases, including UV examination and skin or nail scrapings. Treatment and prevention involve washing the feet daily, drying the feet thoroughly, and wearing cotton socks and breathable shoes. Medical treatment includes antifungal creams, ointments, or tablets prescribed by a doctor. Early treatment is essential to prevent complications, especially for individuals with underlying health conditions. If you suspect you have athlete’s foot, it is strongly suggested that you make an appointment with a podiatrist for a diagnosis and treatment plan.
Athlete’s foot is an inconvenient condition that can be easily reduced with the proper treatment. If you have any concerns about your feet and ankles, contact Dr. George Yarnell from Pennsylvania. Our doctor will treat your foot and ankle needs.
Athlete’s Foot: The Sole Story
Athlete's foot, also known as tinea pedis, can be an extremely contagious foot infection. It is commonly contracted in public changing areas and bathrooms, dormitory style living quarters, around locker rooms and public swimming pools, or anywhere your feet often come into contact with other people.
Solutions to Combat Athlete’s Foot
Athlete’s foot can cause many irritating symptoms such as dry and flaking skin, itching, and redness. Some more severe symptoms can include bleeding and cracked skin, intense itching and burning, and even pain when walking. In the worst cases, Athlete’s foot can cause blistering as well. Speak to your podiatrist for a better understanding of the different causes of Athlete’s foot, as well as help in determining which treatment options are best for you.
If you have any questions please feel free to contact our office located in Lansdowne, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.
Athlete’s foot is a type of fungal infection that affects the skin on the feet. It is caused when the tinea fungus grows on the foot. It is possible to catch the fungus through direct contact with someone who has it or by touching a surface that is contaminated with it. This type of fungus thrives in warm, moist environments such as showers, locker room floors, and swimming pools. Your risk of getting it may also increase by wearing tight-fitting, closed-toe shoes, or by having sweaty feet.
Symptoms of athlete’s foot include itching, stinging or burning sensations between the toes. You may also experience toenails that are discolored, thick, crumbly, or toenails that pull away from the nail bed.
Your podiatrist may diagnose athlete’s foot by detecting these symptoms or by doing a skin test to see if there is a fungal infection present. The most common exam used to detect Athlete’s foot is a skin lesion potassium hydroxide exam. To use this method, your doctor will scrape off a small area of the infected skin and place it into potassium hydroxide. The potassium hydroxide will destroy the normal cells and leave the fungal cells untouched so that they are visible under a microscope.
There are a variety of treatment options for athlete’s foot. Some medications are miconazole (Desenex), terbinafine (Lamisil AT), clotrimazole (Lotrimin AF), butenafine (Lotrimin Ultra), and tolnaftate (Tinactin). While these options may be able to treat your fungus, it is best that you consult with a podiatrist in order to see which treatment option may work best for you.
In some cases, Athlete’s foot may lead to complications. A severe complication would be a secondary bacterial infection which may cause your foot to become swollen, painful, and hot.
There are ways that you can prevent athlete’s foot. Washing your feet with soap and water each day and drying them thoroughly is an effective way to prevent infections. You also shouldn’t share socks, shoes, or towels with other people. It is crucial that you wear shower sandals in public showers, around swimming pools, and in other public places. Additionally, you should make sure you wear shoes that can breathe and change your socks when your feet become sweaty. If you suspect that you have Athlete’s foot, you should seek help from a podiatrist as soon as possible.

A broken foot can abruptly halt your daily routine and mobility, often resulting from traumatic injuries, falls, or repetitive stress. Recognizing the signs is pivotal in seeking prompt treatment. Common symptoms can include acute pain, swelling, bruising, and difficulty bearing weight. If you suspect a break, getting a medical evaluation via X-rays or scans is essential for accurate diagnosis. Treatment options can vary based on the severity and location of the fracture. Mild cases may necessitate immobilization with a cast or brace accompanied by rest and elevation. Severe fractures may demand surgical intervention to realign bones. Physical therapy aids rehabilitation, restoring strength and flexibility. Patience is key, as recovery may take several weeks to months. Prioritizing medical guidance from a podiatrist ensures optimal healing, paving the way for a steady return to an active life. If you have broken your foot, it is suggested that you visit a podiatrist who can offer treatment methods that are right for you.
A broken foot requires immediate medical attention and treatment. If you need your feet checked, contact Dr. George Yarnell from Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
Broken Foot Causes, Symptoms, and Treatment
A broken foot is caused by one of the bones in the foot typically breaking when bended, crushed, or stretched beyond its natural capabilities. Usually the location of the fracture indicates how the break occurred, whether it was through an object, fall, or any other type of injury.
Common Symptoms of Broken Feet:
Those that suspect they have a broken foot shoot seek urgent medical attention where a medical professional could diagnose the severity.
Treatment for broken bones varies depending on the cause, severity and location. Some will require the use of splints, casts or crutches while others could even involve surgery to repair the broken bones. Personal care includes the use of ice and keeping the foot stabilized and elevated.
If you have any questions please feel free to contact our office located in Lansdowne, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.