
Lansdowne, PA
(610) 626-3338

Lansdowne, PA
(610) 626-3338
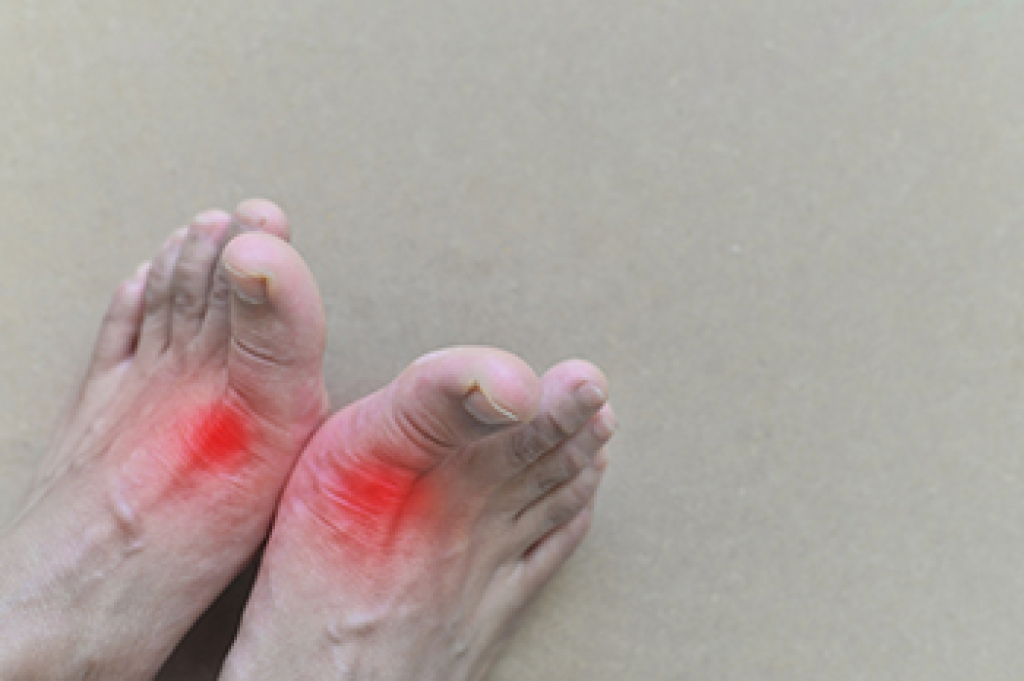
Gout is a form of arthritis characterized by sudden, intense pain and inflammation in the joints, most commonly affecting the big toe. It occurs when uric acid, a waste product from the breakdown of purines in food, builds up in the blood and forms sharp crystals in the joints. There are several causes of gout, including genetics, obesity, excessive alcohol consumption, and a diet high in purine-rich foods such as red meat and seafood. Certain medical conditions like high blood pressure, diabetes, and kidney disease can also increase the risk. When uric acid crystals accumulate in the joints, they trigger an inflammatory response, leading to swelling, redness, and severe pain. Over time, repeated gout attacks can damage the affected joints, causing long-term issues such as joint deformity and reduced mobility. If you have had one or more gout attacks, it is suggested that you consult a podiatrist who can help you to manage this uncomfortable condition.
Gout is a foot condition that requires certain treatment and care. If you are seeking treatment, contact Dr. George Yarnell from Pennsylvania. Our doctor will treat your foot and ankle needs.
What Is Gout?
Gout is a type of arthritis caused by a buildup of uric acid in the bloodstream. It often develops in the foot, especially the big toe area, although it can manifest in other parts of the body as well. Gout can make walking and standing very painful and is especially common in diabetics and the obese.
People typically get gout because of a poor diet. Genetic predisposition is also a factor. The children of parents who have had gout frequently have a chance of developing it themselves.
Gout can easily be identified by redness and inflammation of the big toe and the surrounding areas of the foot. Other symptoms include extreme fatigue, joint pain, and running high fevers. Sometimes corticosteroid drugs can be prescribed to treat gout, but the best way to combat this disease is to get more exercise and eat a better diet.
If you have any questions, please feel free to contact our office located in Lansdowne, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.
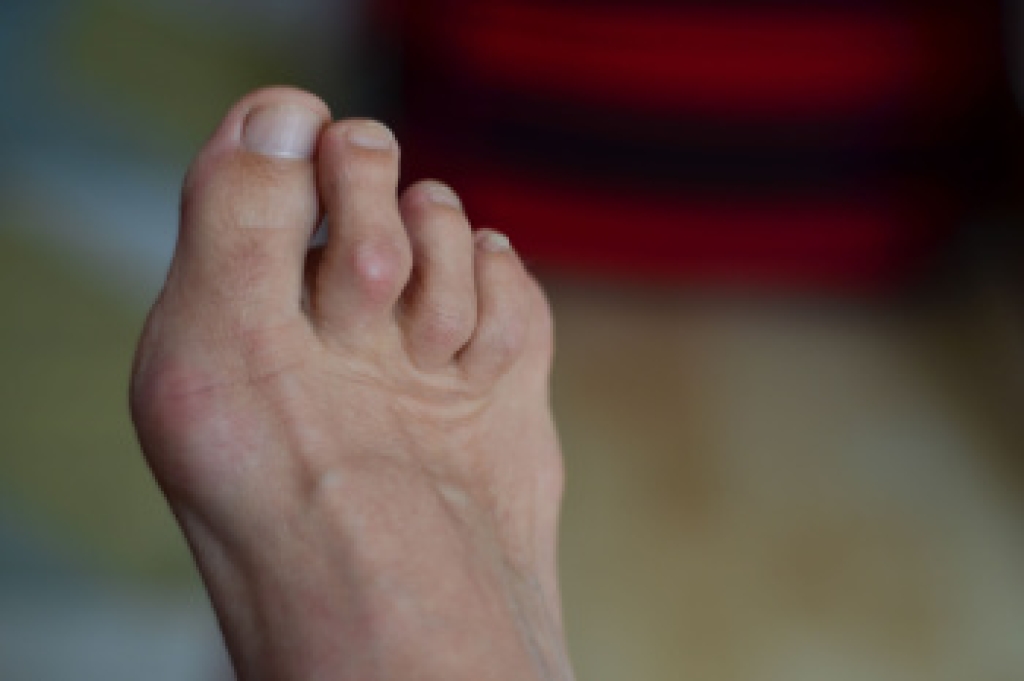
Hammertoe occurs when one or more of the smaller toes become bent in a Z-shaped position, due to an imbalance in the tendons or poor joint alignment. Common causes of hammertoe include wearing ill-fitting shoes, having unusually long toes or metatarsal bones, or conditions like rheumatoid arthritis. The second toe is most frequently affected, but the third and fourth toes can also develop into a hammertoe. This deformity often results in discomfort when wearing shoes, especially those with a narrow or low-toe box. Excessive friction on top of the affected toe can lead to calluses, corns, or even ulcers. In some cases of hammertoe, pain in the ball of the foot, known as metatarsalgia, develops. A podiatrist can diagnose hammertoe through an examination of the foot while assessing other joints for arthritis or other underlying conditions. Treatment options include custom orthotics to reduce pain or surgical correction for rigid deformities. If you have developed a hammertoe that is causing discomfort, it is suggested that you make an appointment with a podiatrist for an exam and treatment options.
Hammertoe
Hammertoes can be a painful condition to live with. For more information, contact Dr. George Yarnell from Pennsylvania. Our doctor will answer any of your foot- and ankle-related questions.
Hammertoe is a foot deformity that affects the joints of the second, third, fourth, or fifth toes of your feet. It is a painful foot condition in which these toes curl and arch up, which can often lead to pain when wearing footwear.
Symptoms
Causes
Genetics – People who are genetically predisposed to hammertoe are often more susceptible
Arthritis – Because arthritis affects the joints in your toes, further deformities stemming from arthritis can occur
Trauma – Direct trauma to the toes could potentially lead to hammertoe
Ill-fitting shoes – Undue pressure on the front of the toes from ill-fitting shoes can potentially lead to the development of hammertoe
Treatment
Orthotics – Custom made inserts can be used to help relieve pressure placed on the toes and therefore relieve some of the pain associated with it
Medications – Oral medications such as anti-inflammatories or NSAIDs could be used to treat the pain and inflammation hammertoes causes. Injections of corticosteroids are also sometimes used
Surgery – In more severe cases where the hammertoes have become more rigid, foot surgery is a potential option
If you have any questions, please feel free to contact our office located in Lansdowne, PA . We offer the newest diagnostic and treatment technologies for all your foot care needs.

Pickleball is a fast-paced, enjoyable sport, but its quick changes in direction and repetitive movements can take a toll on the feet. Players often make sudden stops, pivots, and sprints, which can put stress on the foot joints and muscles. The repetitive nature of the sport can lead to foot pain, especially in the arches, heels, and balls of the feet. Improper footwear is a common cause of foot discomfort, as shoes that lack proper support, cushioning, or stability can worsen the strain on the feet. Additionally, failing to warm up properly before playing pickleball can increase the risk of injury, as muscles and tendons are not fully prepared for the intensity of the movements. To prevent foot pain, it is essential to wear shoes specifically designed for pickleball, practice proper warm-up routines, and listen to your body when it signals discomfort. If you have foot or ankle pain from playing pickleball, it is suggested that you promptly consult a podiatrist who can help you with effective relief and treatment solutions.
Sports related foot and ankle injuries require proper treatment before players can go back to their regular routines. For more information, contact Dr. George Yarnell of Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
Sports Related Foot and Ankle Injuries
Foot and ankle injuries are a common occurrence when it comes to athletes of any sport. While many athletes dismiss the initial aches and pains, the truth is that ignoring potential foot and ankle injuries can lead to serious problems. As athletes continue to place pressure and strain the area further, a mild injury can turn into something as serious as a rupture and may lead to a permanent disability. There are many factors that contribute to sports related foot and ankle injuries, which include failure to warm up properly, not providing support or wearing bad footwear. Common injuries and conditions athletes face, including:
Sports related injuries are commonly treated using the RICE method. This includes rest, applying ice to the injured area, compression and elevating the ankle. More serious sprains and injuries may require surgery, which could include arthroscopic and reconstructive surgery. Rehabilitation and therapy may also be required in order to get any recovering athlete to become fully functional again. Any unusual aches and pains an athlete sustains must be evaluated by a licensed, reputable medical professional.
If you have any questions please contact our office located in Lansdowne, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.

Musculoskeletal conditions of the foot and ankle, such as arthritis, tendonitis, and deformities like bunions or flat feet, often evolve gradually but can significantly challenge the quality of life. These conditions frequently arise from wear and tear, injury, genetic predisposition, or underlying issues like diabetes or obesity. Over time, inflammation, joint damage, or altered biomechanics can lead to pain, stiffness, and reduced mobility. Simple activities like walking or standing may become difficult, limiting independence and daily function. As symptoms progress, compensatory gait changes can strain other joints, leading to knee, hip, or back pain. Chronic discomfort may also impact mental well-being. If you have foot or ankle pain, it is suggested that you visit a podiatrist for a prompt diagnosis and treatment to avoid negative effects on the quality of your life.
Arthritis can be a difficult condition to live with. If you are seeking treatment, contact Dr. George Yarnell from Pennsylvania. Our doctor can provide the care you need to keep you pain-free and on your feet.
Arthritic Foot Care
Arthritis is a joint disorder that involves the inflammation of different joints in your body, such as those in your feet. Arthritis is often caused by a degenerative joint disease and causes mild to severe pain in all affected areas. In addition to this, swelling and stiffness in the affected joints can also be a common symptom of arthritis.
In many cases, wearing ill-fitting shoes can worsen the effects and pain of arthritis. Wearing shoes that have a lower heel and extra room can help your feet feel more comfortable. In cases of rheumatoid arthritis, the arch in your foot may become problematic. Buying shoes with proper arch support that contour to your feet can help immensely.
Alleviating Arthritic Pain
It is best to see your doctor for the treatment that is right for your needs and symptoms. Conditions vary, and a podiatrist can help you determine the right method of care for your feet.
If you have any questions please feel free to contact our office located in Lansdowne, PA . We offer the newest diagnostic tools and technology to treat your foot and ankle needs.